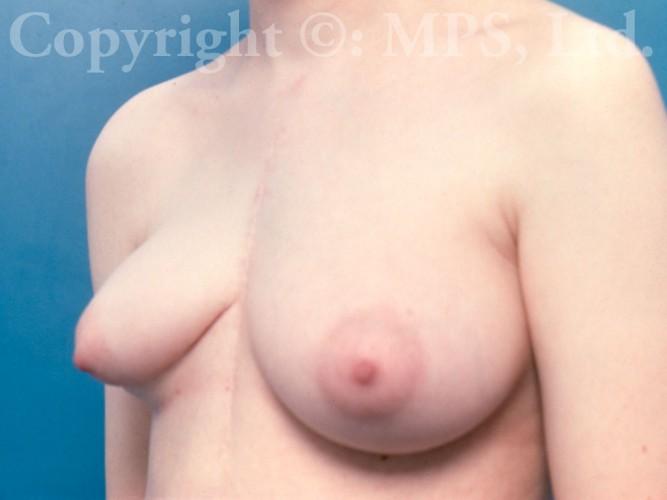
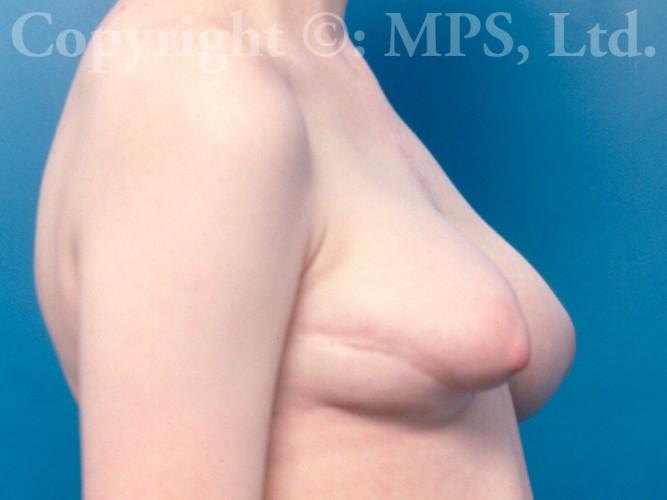
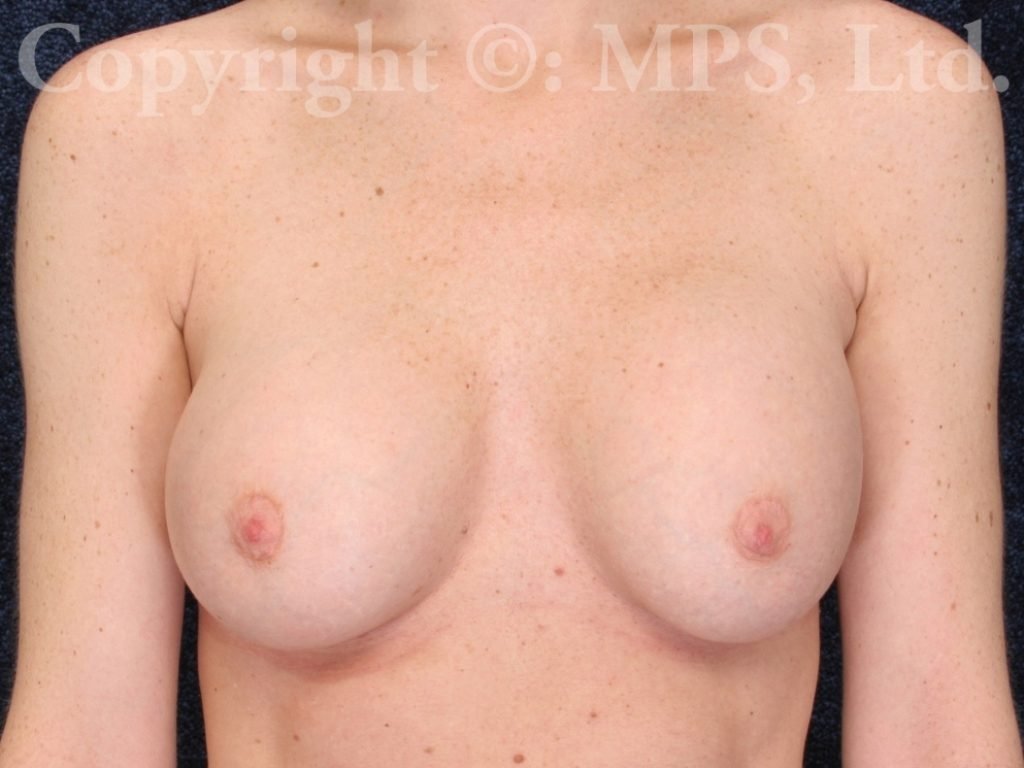
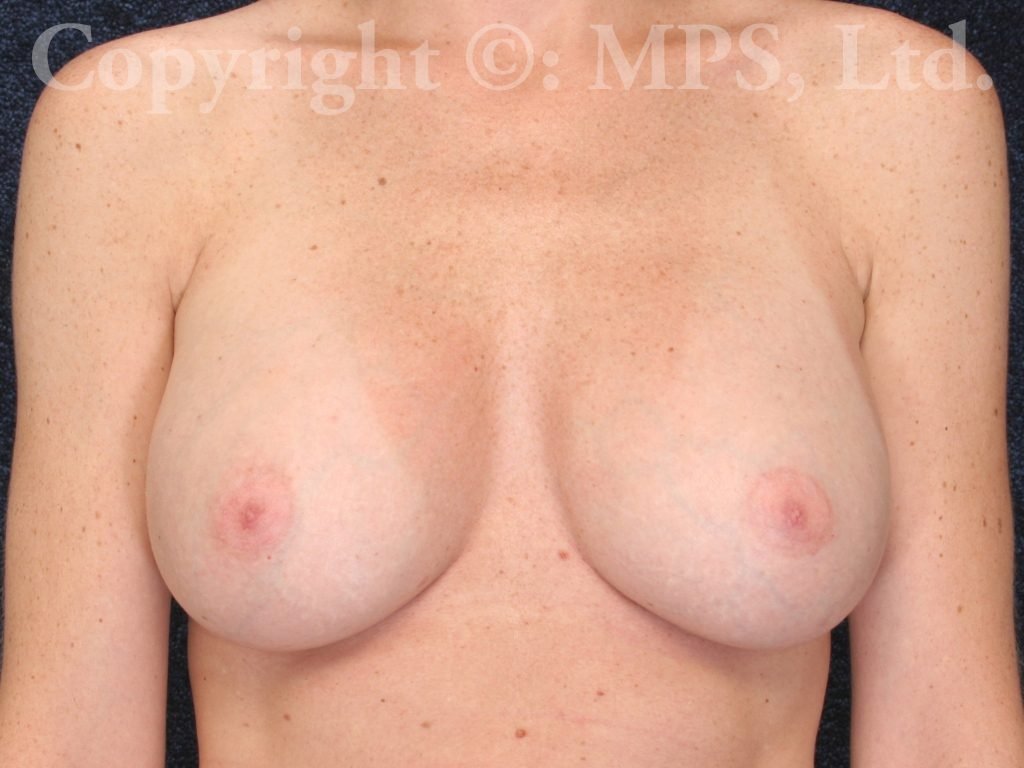
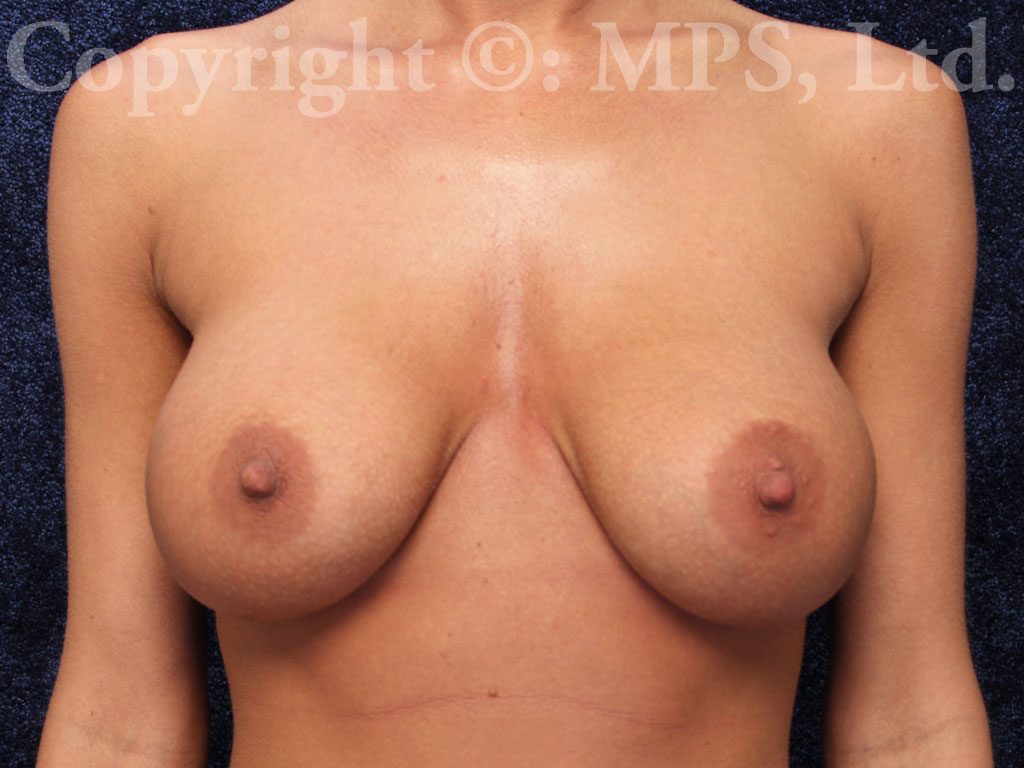
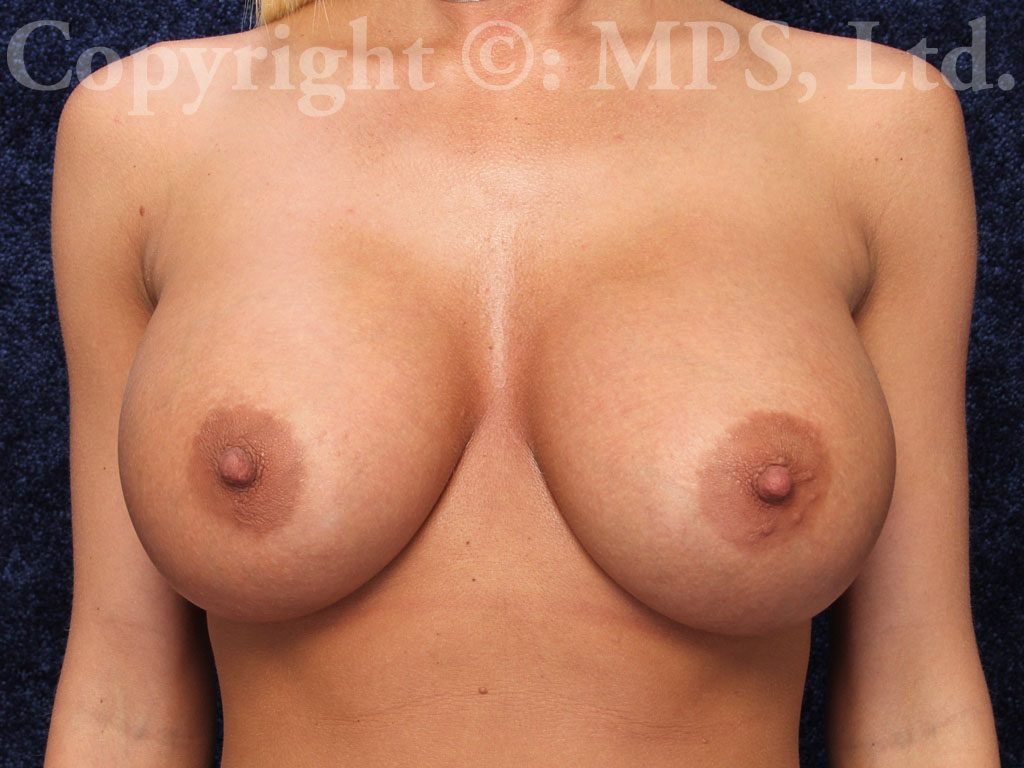
Breast Implant Revision
Some women who undergo breast enlargement surgery are dissatisfied with the final appearance of their breasts or can experience unwanted complications such as saline implant deflation, malposition, or capsular contracture (hardness). Breast augmentation revision surgery is offered at Minneapolis Plastic Surgery, LTD. in Minnesota to yield a more natural and soft breast appearance. What is involved in each surgery depends on the individual treatment needed, but our final goal is always the same — to restore the positive self-image of our patients.
Candidates for Breast Augmentation Revision Surgery
Women interested in corrective breast surgery have had their breasts augmented surgically but are dissatisfied with their results or have experienced complications. They may want their implants to be replaced or removed entirely. Our American Board of Plastic Surgery-certified plastic surgeons Dr. Richard H. Tholen and Dr. Douglas L. Gervais have extensive experience in correcting breast augmentation problems, often in patients who received their surgery elsewhere and do not wish to return to their initial surgeon. Since no surgeon is “perfect” and cannot truthfully boast of “no complications,” this can occur in a few of our own patients as well. Our experience in improving the results of patients with problems after breast implants has decreased the incidence of these problems in our own patients. The reasons for breast augmentation revision may include any of the following:
- Breast asymmetry, Poland’s Syndrome, or Tuberous Breasts
- Dissatisfaction with the size, shape, or feel of breasts
- Results that do not look natural, or are out of proportion
- Switch from saline to silicone implants (or from silicone to saline implants)
- Capsular Contracture (tight or painful scar around implants, often causing firmness or distortion)
- Implant rupture, deflation, or leakage (saline)
- Infection
- Malposition or shifting of implants (double bubble; too-low or too-high crease)
- Symmastia (loss of cleavage), often termed “uni-boob” or “breadloafing”
- Wrinkling of the implants (most commonly saline)
- Unsatisfactory external scars
- Persistent ptosis (sagging or droop) requiring breast lift
Not every implant problem is able to be completely corrected, but virtually every one can be improved, sometimes substantially. With over 55 combined years of experience with literally thousands of saline and silicone breast augmentation patients, our American Board of Plastic Surgery-certified plastic surgeons can assess your concerns, formulate a precise surgical plan, and carefully operate with specific goals in mind. More than one re-operation may be necessary in challenging cases.
Problems after breast augmentation can occur in any patient, and with any plastic surgeon. The best breast augmentation surgeons are those who have not only years of experience in improving poor outcomes from other doctors, but also have learned to incorporate that experience to minimize the potential for those same problems in our own patients. For more details about elective breast enlargement surgery, click on the highlighted link.
WARNING:
This gallery contains nudity not suitable for those under 18 years of age. By viewing you acknowledge this warning
Procedure
Prior to consideration of any surgery, our American Board of Plastic Surgery-certified plastic surgeons with over 55 combined years of breast augmentation experience will carefully examine you, identify your concerns and anatomic or implant issues, and review options and make recommendations. These recommendations are based on extensive experience with breast surgery of all kinds, and may require removal or replacement of implants. In many cases, breast revision surgery can be done through already-existing scars. Unsightly or misplaced scars may be revised or removed entirely.
A pre-operative history and physical examination by your family doctor, internist, or gynecologist is necessary to ensure the safest possible conditions for anesthesia and surgery. This should be completed within two weeks prior to your breast implant revision surgery. You should also avoid aspirin or ibuprofen-containing products, as well as any tobacco or nicotine products, for a minimum of two weeks prior to surgery. You will need someone to bring you home after discharge who will also stay with you the entire night after your operation, and who can bring you back to the office for recheck the following day when recommended.
In cases where implants require removal, the internal scar tissue surrounding the old implants (capsule) may be removed along with the breast implants. Women who have their breast implants removed or implant size decreased may need to consider breast lift surgery to create a shapelier look and counteract any deflation or sagging that may result. These procedures can, in virtually all cases, be safely performed in Minneapolis Plastic Surgery’s nationally-accredited (AAAASF) on-site breast surgery center.
While many patients hope that touch-up or revisionary surgery will be less serious or complicated than the original surgery, with more rapid and less uncomfortable recovery, secondary surgery actually often presents significantly more challenging problems and anatomic considerations to be understood and skillfully dealt with. This is not “quick and easy” surgery; rather, it often requires more adroit technique, operative time, and breast surgery experience to satisfactorily improve the issues that arise from poor outcomes obtained elsewhere.
Recovery and Results
For any woman having breast revision surgery, the recovery period and activity limitations will be similar (not less) to the recovery after her first breast surgery, even when post-operative discomfort is less. Patients should refrain from exercise and heavy lifting for several weeks. Detailed instructions are given to all patients after surgery to guide them through the recovery process. Some patients may require more than one operation, and not every problem has an easy solution, but the plastic surgeons at Minneapolis Plastic Surgery, LTD. have over 55 years of combined experience with many patients who have had less than ideal outcomes elsewhere. No surgeon (anywhere) should offer guarantees, nor should patients ever feel their payment is for a specified outcome or result. You should seek careful examination and measurements, thoughtful and experienced analysis, detailed recommendation, and skillful surgical technique, which is what you receive at Minneapolis Plastic Surgery, LTD. Though this does not guarantee a desired result, this approach offers the highest likelihood of success and the outcome we strive for.
Cost of Breast Implant Revision Surgery
Breast implant revision can be as simple as local anesthesia implant exchange, for which total cost may be even less than initial breast augmentation (around $7500—saline or $8500—silicone). If your original surgery was performed by our plastic surgeons, surgeon’s fees for revisionary surgery are often reduced or waived; however, implant, operating room (and anesthesia fees, if requested or necessary) are each patient’s responsibility.
Revision of breast lift plus implants, treatment of tuberous breasts, or surgery for capsular contracture are examples of revisionary operations that are often much more complex than the initial surgery, and costs are correspondingly higher. Each of the many conditions and reasons for revision discussed above are as individual as each patient’s unique situation; personal examination is necessary in each case to identify the problem(s) and determine the appropriate surgical plan for treatment, as well as the amount of operating room time needed to complete the surgery. Exact costs are available at the time of complimentary consultation with our American Board of Plastic Surgery-certified plastic surgeons. The most complex revisions can cost $9000-$15,000 or more, depending on the severity of the problem. Financing options are available.
Because of the high demand for free consultations with our plastic surgeons, our staff will ask for a credit card number in order to schedule a consultation; there is no charge whatsoever for appointments that are kept–you will be charged $100 only if you fail to keep a scheduled appointment, or fail to cancel at least 48 hours in advance of your appointment time–for Monday appointments, you must cancel no later than noon on the previous Thursday.